Healthcare Data Exchange Challenges
The Role of APIs in Facilitating Seamless Data Integration
Benefits of Using APIs Integration for Healthcare Data Exchange
API Integration and Data Standards: The Foundation for Interoperability
Thank you for reaching out to Sigma Software!
Please fill the form below. Our team will contact you shortly.
Sigma Software has offices in multiple locations in Europe, Northern America, Asia, and Latin America.

USA

Sweden

Germany

Canada

Israel

Singapore

UAE

Australia

Austria

Ukraine

Poland

Argentina

Brazil

Bulgaria

Colombia

Czech Republic

Hungary

Mexico

Portugal

Romania

Uzbekistan
Seamless data exchange between different systems and healthcare providers is essential to ensure timely, accurate, and comprehensive patient care. This article explores how API integration in healthcare overcomes challenges and enables seamless data exchange.
Healthcare Data Exchange Challenges
The Role of APIs in Facilitating Seamless Data Integration
Benefits of Using APIs Integration for Healthcare Data Exchange
API Integration and Data Standards: The Foundation for Interoperability
Key Highlights:
By adopting API integration and adhering to data standards, healthcare organizations can create a more connected and data-driven healthcare ecosystem, ultimately improving patient care and operational efficiency.

While the potential benefits of seamless healthcare data exchange are significant, several challenges stand in the way:
Healthcare data is often stored in siloed systems that don’t communicate effectively with each other. This lack of interoperability results in fragmented patient records, making it difficult to provide comprehensive patient care.
Solution: Invest in Healthcare Information Exchange (HIE) platforms that act as intermediaries and facilitate the exchange of data between disparate systems. Encourage the adoption of interoperability standards such as HL7 and FHIR to ensure that systems can communicate effectively.
The lack of standardized communication methods makes it difficult to exchange data seamlessly. As a result, data is exchanged in a variety of formats and structures, leading to confusion and inefficiency.
Solution: Establish clear data exchange protocols and standards within your organization. Encourage providers to adopt standardized data exchange formats. Consider adopting Health Level Seven (HL7) or Fast Healthcare Interoperability Resources (FHIR) standards to ensure consistent communication.
The success of data exchange doesn’t guarantee its quality. Inaccurate, outdated, or incomplete data can jeopardize patient care, underlining the importance of consistent, reliable information across systems.
Solution: Implement data governance practices to ensure data accuracy and integrity. Regularly audit and cleanse data to eliminate inaccuracies. Use data validation and verification tools to maintain data quality.
Integrating various systems, especially legacy systems, presents complex technical obstacles. These include different data models and complications in establishing seamless connectivity.
Solution: Invest in integration platforms and middleware solutions that can bridge the gap between systems with different data models. Use data transformation tools to convert data into compatible formats. Consider incremental system upgrades to modernize legacy systems.
Regulatory compliance is the most significant challenge in healthcare, encompassing a complex web of regulations aimed at patient safety. Healthcare providers must comply with numerous regulations, including data security and patient confidentiality.
Solution: Implement Application Programming Interfaces (APIs) that comply with healthcare data exchange standards and incorporate robust security measures. Ensure that your systems encrypt data both at rest and in transit. Conduct regular security audits and risk assessments to identify and address vulnerabilities.
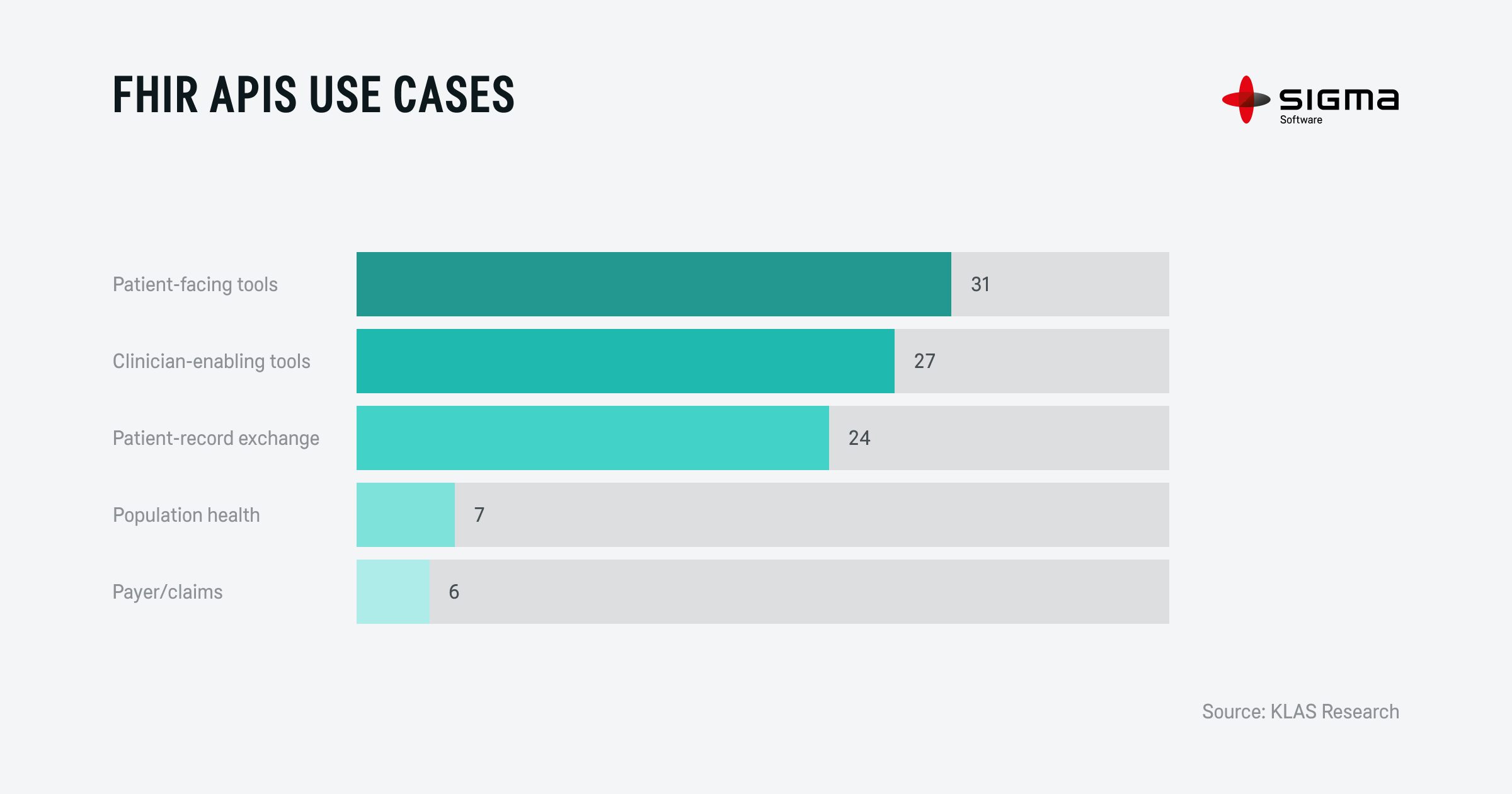
In healthcare, where various systems, applications, and devices coexist, API integration is critical to enabling seamless data exchange. According to KLAS Research 2021 report, the adoption of APIs introduces new ways to enable data exchange across a wide range of use cases. This standardized method of communication breaks down data silos, ensuring that vital patient information is accessible across different healthcare organizations. Whether it’s sharing patient records between hospitals, enabling wearable devices to sync with EHRs, or connecting diagnostic tools for real-time analysis, APIs streamline data exchange and improve the efficiency of the entire healthcare ecosystem.
The adoption of API integration in healthcare offers numerous benefits that contribute to improved patient care, increased operational efficiency, and accelerated innovation:
API integration bridges the gap between disparate systems, promoting interoperability, and empowering healthcare providers with timely, accurate, and comprehensive patient information. As the healthcare industry continues to embrace digital transformation, APIs will undoubtedly play a critical role in shaping the future of healthcare data exchange.
In the dynamic world of modern healthcare, achieving seamless interoperability between disparate systems is critical to delivering efficient and patient-centered care. This is precisely where API standards come in, serving as the foundational framework that enables different healthcare applications, devices, and platforms to communicate effectively. These standards provide a common language that bridges the gap between disparate systems, facilitating the exchange of critical health information while maintaining data integrity, security, and accuracy:
FHIR is a transformative API standard that uses modern web principles to enable seamless data exchange. Its RESTful architecture, combined with standardized resources, facilitates the exchange of structured healthcare information. FHIR is ideal for scenarios where real-time access to patient data is critical, such as clinical decision support systems and patient portals. For more detailed information on this standard, you can read this article.
Designed for medical imaging, DICOMweb extends the traditional DICOM standard to web-based interactions. It’s essential for exchanging medical images, reports, and related information between different imaging systems, supporting radiology departments, and diagnostic services.
It combines the robustness of FHIR with an authorization framework that enables secure access to electronic health records. This standard is best suited for developing interoperable healthcare applications that seamlessly integrate with electronic health record systems to improve clinical decision making and patient care.
CCDA focuses on the exchange of patient summary documents such as discharge summaries and progress notes. It defines structured formats for clinical documents, making them suitable for sharing essential patient information across care settings.
Similar to CCDA, CDA defines document structures for the exchange of clinical information. It’s valuable when more complex clinical documents need to be shared between different systems.
IHE promotes the adoption of established standards to achieve interoperability in healthcare IT systems. It’s particularly useful for guiding the implementation of standards in specific use cases and solving practical healthcare challenges.
Although older, HL7 v2.x is still widely used for messaging between systems, particularly for administrative purposes. It’s suitable where more advanced standards such as FHIR have not yet been adopted.
Incorporating an appropriate API standard depends on the specific healthcare use case and data exchange requirements. Organizations should carefully evaluate their needs, existing infrastructure, and future goals to select the appropriate API standard that aligns with their interoperability objectives. Together, these standards collectively pave the way for improved data exchange, better patient care, and a more connected healthcare ecosystem.
In the digital age of healthcare, seamless data exchange is critical to delivering optimal patient care. API integration is emerging as the solution to overcome the challenges of data silos, interoperability issues, and security concerns. Standardized API protocols provide the foundation for interoperability, enabling different systems to communicate seamlessly.
By implementing API standards and promoting interoperability, the healthcare sector can achieve improved data exchange, better patient care, and operational excellence.
If you are considering improving your healthcare software through data exchange and API integrations or have questions about healthcare solutions, please contact our experts. They are ready to provide you with the answers you need to make informed decisions.
At our custom healthcare software development company, we specialize in creating innovative solutions that improve the efficiency of healthcare systems. As a leading healthcare software development company, we offer world-class healthcare software development services tailored to your specific needs. Partnering with our dedicated team ensures that you have access to bespoke solutions that meet your unique requirements, and that will drive your healthcare system into the future.

Andrii's expertise primarily encompasses the Healthcare industry. Bolstered by extensive knowledge in the Information Security domain and ML/AI. Andrii Pastushok is committed to guaranteeing clients receive an exceptional product development experience.
Linkedin profileHealthcare Data Exchange Challenges
The Role of APIs in Facilitating Seamless Data Integration
Benefits of Using APIs Integration for Healthcare Data Exchange
API Integration and Data Standards: The Foundation for Interoperability


For decades, the manufacturing formula for success was the same – build great equipment, ship to the Client, and get the profit. Now, more OEMs are discovering ...

If you own a product line, run an embedded or connectivity team, or look after the cloud and data stack for connected devices, the EU Data Act probably didn’t a...

At Sigma Software, we constantly explore how emerging technologies can amplify engineering efficiency. Recently, a team from Sigma Software that develops Dovkol...
Would you like to view the site in German?
Switch to German