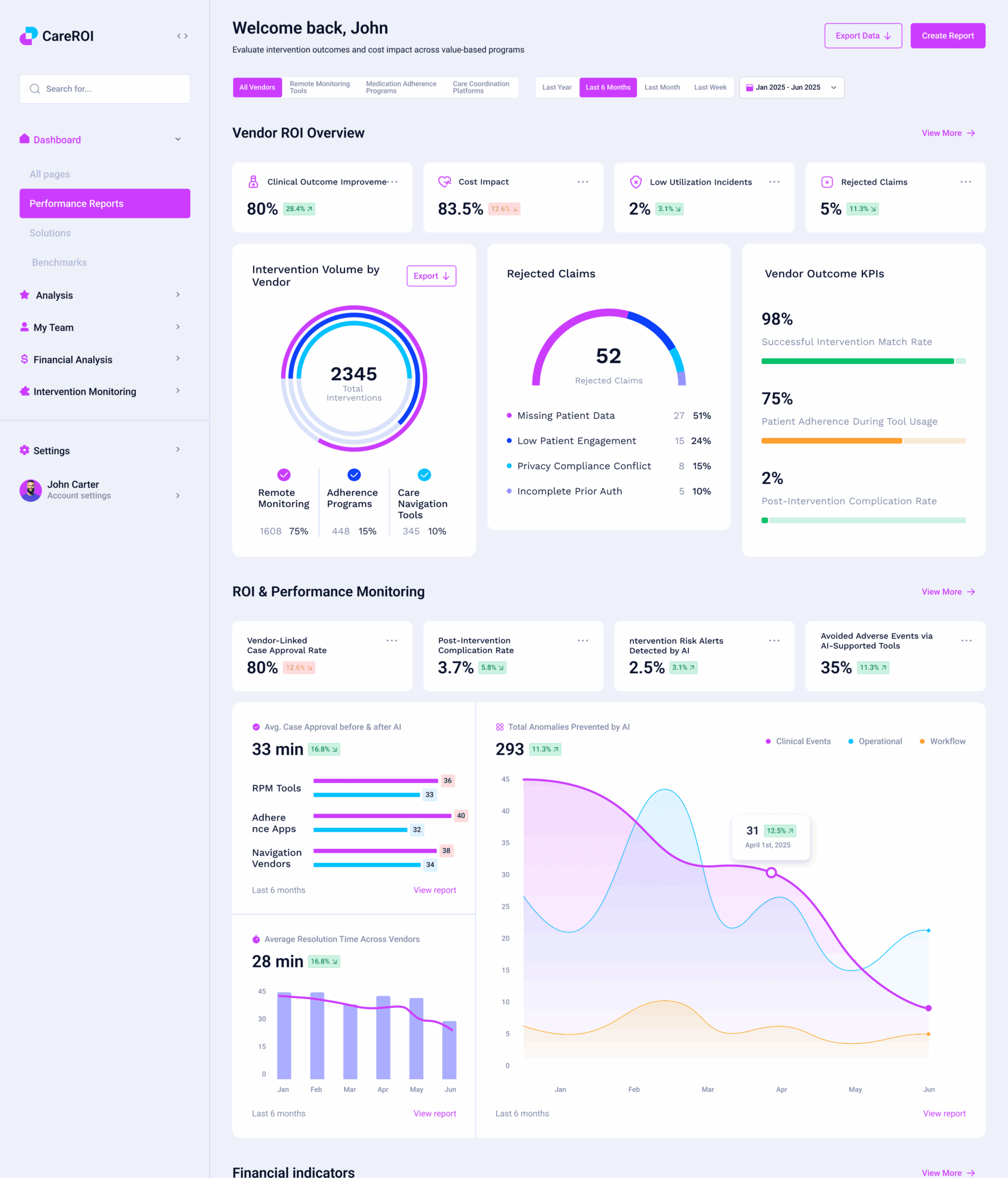
Why Keep Historical Value-based Care Data?
What a Healthcare Data Analytics Platform Must Deliver for Value-based Care
Health Care Data Analytics, ML, and KPI Operationalization
Governance, Privacy & Compliance for Healthcare Data Analytics Platforms
Problems that a Custom Healthcare Analytics Platform Can Solve
Value-based Care Data Analytics Implementation Roadmap
Procurement Checklist for CTOs: Custom Healthcare Data Analytics Solutions vs. Managed Services
Choosing the Right Healthcare Data Analytics Platform Partner